Multiple Insulinoma of Pancreas in MEN 1 Syndrome - A Rare Case
- ivyhpbgigensurg
- Jan 15
- 4 min read
Updated: Feb 5
A young lady presented with increased appetite, weight gain and episodes of hypoglycemia, i.e. ghabrahat, sweating, etc. Multiple consults from various doctors, Cect and MRI diagnosed a very rare disease for which the patient visited us. After a thorough evaluation of disease localisation, the patient was planned for surgery.
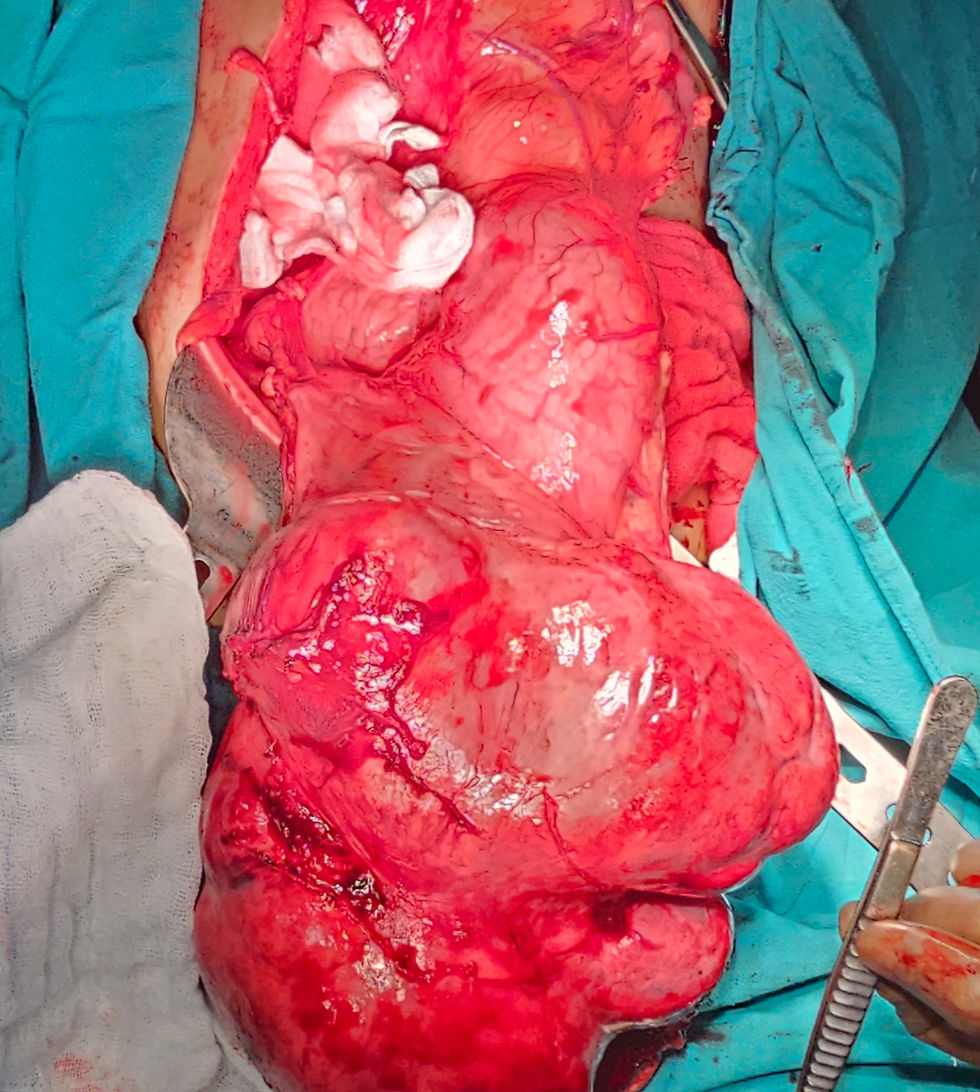
The patient underwent a successful surgery with enucleation of multiple pancreatic insulinomas with intraoperative ultrasonography, intraoperative frozen section and pathological examination to confirm cure during surgery.
The patient was cured of the disease and is on follow-up.
MEN 1 Syndrome and Insulinoma
What is MEN 1 Syndrome?
MEN 1 syndrome (Multiple Endocrine Neoplasia type 1) is a rare inherited condition in which a person develops tumors or overgrowth in certain hormone-producing glands of the body.
These tumors are usually not cancer, but they can cause problems because they make too many hormones.
Which parts of the body are affected?
MEN 1 mainly affects three glands (doctors often remember it as the “3 P’s”):
1. Parathyroid glands (neck)
These glands control calcium levels in the blood
In MEN 1, they become overactive
This causes high calcium levels
Common symptoms:
Kidney stones
Bone pain or fractures
Tiredness
Abdominal pain
Depression or mood changes
2. Pancreas (digestive hormone tumors)
Small tumors can form in the pancreas
They may produce excess hormones like insulin or gastrin
Problems that can happen:
Low blood sugar → sweating, shakiness, fainting
Excess stomach acid → ulcers, stomach pain, vomiting
3. Pituitary gland (brain)
The pituitary controls many body hormones
Tumors here may increase hormone production
Symptoms may include:
Headache
Vision problems
Milk discharge from breast (even in men)
Irregular periods in women
Sexual problems or infertility
Why does MEN 1 happen?
MEN 1 is caused by a gene defect
It is passed from parents to children
If one parent has MEN 1, there is a 50% chance the child may have it
How is MEN 1 diagnosed?
Doctors may suspect MEN 1 when:
A person has tumors in more than one endocrine gland
There is a family history
Tests include:
Blood tests (hormone levels, calcium)
Imaging scans (CT, MRI)
Genetic testing
How is MEN 1 treated?
There is no permanent cure, but the condition can be well controlled.
Treatment includes:
Surgery to remove problematic glands or tumors
Medicines to control hormone levels
Regular follow-up and screening for life
Important points to remember
MEN 1 is long-term, but manageable
Early diagnosis prevents serious complications
Family members may also need testing
Regular medical check-ups are very important
What is an insulinoma?
An insulinoma is a small tumor of the pancreas that makes too much insulin.
Insulin is the hormone that lowers blood sugar.When too much insulin is produced, the blood sugar falls dangerously low.
How is insulinoma related to MEN 1?
MEN 1 syndrome causes multiple hormone-producing tumors
In MEN 1, insulinomas:
Occur at a younger age
Are often multiple (more than one tumor)
May come back even after treatment
What problems does insulinoma cause?
Because insulin is high, blood sugar becomes low (hypoglycemia).
Common symptoms include:
Sweating
Shakiness or tremors
Hunger
Palpitations
Headache
Confusion or strange behavior
Blurred vision
Fainting or seizures (in severe cases)
Symptoms often:
Occur during fasting
Improve after eating sugar or food
Typical warning sign (important clue)
Doctors use something called Whipple’s triad:
Symptoms of low blood sugar
Low blood sugar measured in blood test
Relief of symptoms after eating or giving glucose
How is insulinoma diagnosed?
Tests may include:
Blood tests showing:
Low blood sugar
High insulin levels at the same time
Fasting test done under medical supervision
Scans like CT, MRI, or special scans to locate the tumor
How is insulinoma treated?
1. Surgery (main treatment)
Removal of the tumor(s) from the pancreas
In MEN 1, multiple tumors may need careful surgical planning
2. Medicines (if surgery is delayed or not possible)
Drugs to prevent low blood sugar
Medications that reduce insulin release
Why is insulinoma in MEN 1 important?
Low blood sugar can be life-threatening
Early diagnosis prevents brain damage and seizures
Lifelong follow-up is needed because tumors can recur
Key points in simple words
Insulinoma is a pancreatic tumor that causes low blood sugar
In MEN 1, insulinomas are often multiple and early in onset
Main symptoms are related to hypoglycemia
Surgery is the best treatment
Regular monitoring is essential

WHY SURGERY FOR MEN 1 SYNDROME AND INSULINOMA
Surgery in MEN 1 Syndrome
1. Parathyroid Surgery
(Most common and usually first surgery)
Almost all MEN 1 patients develop overactive parathyroid glands
Surgery involves removing most or all parathyroid glands
Types of surgery:
Removal of 3½ glands (leaving a small part)
Or removal of all glands with re-implantation of tissue elsewhere
Outcome:
Calcium levels usually return to normal
Bone pain and kidney stones improve
2. Pancreatic Surgery (for Insulinoma)
What is done?
The surgeon removes the tumor(s) from the pancreas
In MEN 1, insulinomas are often multiple, so surgery may include:
Removal of part of the pancreas
Removal of visible tumors
Goal of surgery:
Stop excess insulin production
Prevent low blood sugar attacks
Outcomes after Insulinoma Surgery
Short-term results:
Blood sugar levels usually return to normal
Symptoms like sweating, shaking, and fainting disappear
Quality of life improves significantly
Long-term results:
Most patients do very well
In MEN 1, insulinomas may come back, so repeat treatment may be needed
Possible Risks of Surgery (Simple Explanation)
Bleeding or infection
Leakage of pancreatic fluid
Temporary or permanent diabetes (rare but possible)
Low calcium after parathyroid surgery
Doctors take steps to minimize these risks.
Follow-Up After Surgery (Very Important)
MEN 1 is a lifelong condition, so regular follow-up is essential, even after successful surgery.
Follow-up includes:
Regular blood tests:
Calcium levels
Blood sugar
Hormone levels
Periodic scans to detect new tumors
Monitoring symptoms like:
Weakness
Low sugar episodes
Bone pain
Family screening:
Close family members may need testing
Genetic counseling is recommended
Long-Term Outlook
Surgery controls symptoms but does not cure MEN 1
With regular monitoring, most patients live a normal and active life
Early detection of new tumors leads to better outcomes
Key Points in Simple Words
Surgery removes problem-causing tumors and glands
Insulinoma surgery prevents dangerous low blood sugar
Symptoms usually improve after surgery
Tumors can return in MEN 1
Lifelong follow-up is essential.


Comments